As more providers look to integrate continuous glucose monitoring into their clinical workflows, the challenge is no longer access to glucose data—it’s implementation at scale. Continuous glucose monitoring (CGM) offers meaningful clinical insight by providing real-time glucose levels through a medical device that measures glucose in the interstitial fluid just under the skin. However, without the right structure, it can introduce operational complexity. Integrating CGM brings the benefit of improved patient outcomes and streamlined workflows for healthcare professionals.
Ashley Koff, founder of the Better Nutrition Program (BNP), has built a model that combines CGM with Theia’s infrastructure to support scalable, data-driven nutrition care. Her approach focuses on how to implement CGM in clinical practice by integrating CGM into existing workflows in a way that improves outcomes without increasing internal burden.
From Traditional Nutrition Practice to a Scalable Model
Q: How would you describe your model today compared to a traditional nutrition practice?
Ashley explains that her model no longer operates as a standalone nutrition service, but as an extension of other providers’ care models.
“When nutrition is referred out, you lose continuity,” she notes. “When it’s integrated, you see better outcomes because it stays within the patient’s experience.”
The Better Nutrition Program was built around that principle—embedding nutrition directly into care delivery rather than layering it on top. This allows providers to offer structured, personalized nutrition support without building additional internal systems.
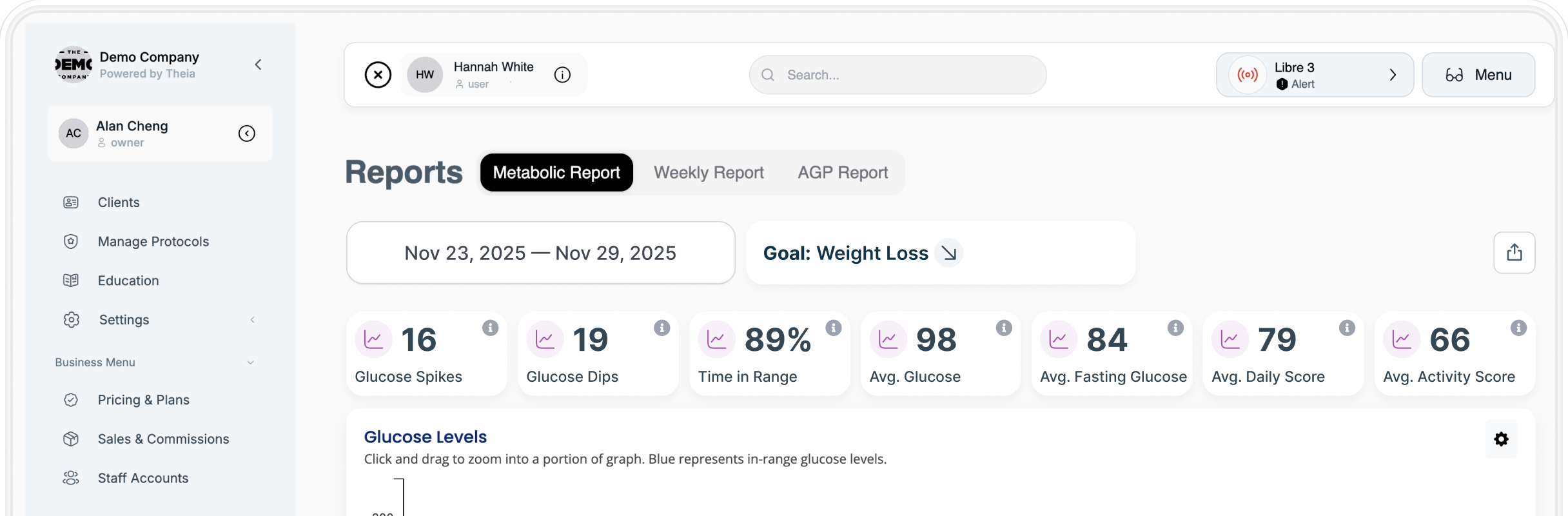
Theia supports this model by enabling consistent CGM delivery and patient experience across practices, removing variability in how the tool is implemented. Theia also provides tools and resources to help providers implement CGM consistently and efficiently across their practices.
Why Nutrition Often Breaks Down in Clinical Workflows
This is where continuous glucose monitoring, particularly when supported by Theia, becomes useful. It allows providers to translate real-time glucose data into clinical decisions rather than relying on assumptions. Effective analysis of CGM data is essential for making informed treatment decisions, as it enables providers to review and interpret historical glucose trends and sensor readings for better patient outcomes.
The Clinical Role of CGM for Providers
Q: What role does CGM play in your model today?
Ashley describes CGM as a visibility tool that fills gaps left by traditional markers. “A1C is an average—it doesn’t tell you what’s actually happening day to day.”
CGM provides continuous, real-time glucose levels to users, as intended, allowing for more precise diabetes management. It tracks how various factors—such as food, stress, sleep, exercise, medication, and illness—influence glucose levels. Through Theia, these responses can be interpreted alongside behavior, giving providers a more complete picture.
“It’s not just about food. You’re seeing how everything is impacting glucose.” Rather than replacing clinical judgment, CGM supports it by making patterns easier to identify and act on.
Why CGMs Require Operational Support
Q: What challenges did you encounter when implementing CGM?
Ashley is clear that the biggest barrier was not clinical.
“The challenge wasn’t the data—it was everything around it.”
Early on, her team managed onboarding, troubleshooting, and device coordination internally. While manageable at a small scale, this quickly became unsustainable. “We had people on the phone with pharmacies, dealing with sensor issues—it added up fast.” Healthcare providers often face additional challenges related to navigating the health care system and meeting insurance requirements for CGM devices. Proper documentation is required for ordering sensors and insurance authorization, which can add to the administrative burden.
Over time, this began to pull focus away from patient care and treatment decision making. Integrating Theia allowed her team to offload these responsibilities.
“With Theia, we’re not managing devices anymore. They handle that, and we can focus on the patient.”
For providers, this separation between operational support and clinical work is what makes CGM scalable. At a certain point, it stops being scalable if your team is managing devices instead of patients.
Watch the Full Conversation
See how Ashley implements CGM using Theia—from onboarding and patient monitoring to clinical decision-making—and what that looks like inside a real practice.
How CGM Data Is Interpreted in Practice
Q: What do you focus on when reviewing CGM data?
Ashley emphasizes that interpretation is not based on a single metric.
“If you try to analyze every number, you’re going to miss the point.”
These glucose patterns are evaluated in the context of behavior—meal composition, timing, sleep, and activity. Evaluation of CGM data can be enhanced using tools like the Ambulatory Glucose Profile (AGP), available in Theia which provides a concise, single-page summary of glucose data to help healthcare professionals quickly identify patterns including glucose variability and time in range.
Using Theia, providers can adjust how they interpret data based on the individual patient’s glucose trends.
“That flexibility matters. You’re not applying the same framework to everyone.”
She reinforces that context is essential.
“Data without context isn’t useful. You have to connect it to what the patient is actually doing.”
From Data to Intervention
Q: How does continuous glucose monitoring influence clinical decision-making?
Ashley explains that CGM improves precision rather than changing the type of intervention.
“The intervention is usually simple—it’s just more precise once you can actually see what’s happening.”
She shares an example of a patient with diabetes who was eating a banana daily based on prior guidance. CGM revealed a significant blood glucose spike.
“We didn’t remove it—we adjusted it.”
By modifying portion size and pairing it with fat, the patient was able to maintain the food while improving glucose stability.
Clinical trials have shown that CGM systems, including Dexcom CGM and other CGM systems, can help reduce A1C levels and minimize problematic hypoglycemia and severe low blood sugar in users, supporting evidence-based adjustments in diabetes management.
“That’s the difference. You’re not guessing—you’re adjusting based on what you can actually see.”
How CGM Improves Patient Adherence
Q: How does continuous glucose monitoring impact patient adherence?
Ashley notes that the primary impact is on understanding.
“It improves adherence because patients can see what’s happening in real time.”
When patients observe how their body responds to food, exercise, stress, and medication, they are more likely to make consistent changes. This shifts the role of the provider.
“You’re not just telling them what to do—you’re helping them interpret their own glucose data.”
Education is crucial for both patients and healthcare professionals to maximize the benefits of CGM; providers are encouraged to participate in diabetes education classes or consult with certified diabetes care and education specialists to learn how to use CGM devices safely and effectively.
Over time, this reduces reliance on motivation and increases long-term consistency in diabetes management.
What Would You Say to a Provider Who’s Sitting Where You Were a Year Ago?
Ashley recommends starting with direct experience. “Go through the process yourself. That’s the fastest way to understand it.” She emphasizes that many healthcare providers underestimate the operational side of continuous glucose monitoring.
“It’s not just about having access to the data—it’s how you deliver it.”
Without the right infrastructure, onboarding, troubleshooting, and device failure management can become a barrier to scaling. “That’s where something like Theia makes a difference. It removes the operational burden so you can focus on patient monitoring.”
For providers evaluating continuous glucose monitoring, the key is not just adoption, but integration—ensuring the tool fits within the realities of primary care and other clinical workflows.
Without a structured system, continuous glucose monitoring can introduce additional complexity. With the right infrastructure, it becomes a tool for improving metabolic health insights, patient engagement, and care precision.
This is where platforms like Theia support healthcare professionals by standardizing CGM delivery, reducing operational overhead, and enabling consistent patient monitoring across different care settings.
Implementing Theia in Clinical Practice
For healthcare providers, implementing CGM in clinical practice requires more than just access to a CGM device. Continuous glucose monitoring in clinical practice involves patient onboarding, device setup, ongoing patient monitoring, and interpretation of blood glucose data over time.
CGMs allow healthcare professionals to monitor glucose levels continuously, track glucose variability, and improve metabolic health outcomes. When used correctly, CGM provides actionable insights into how patients respond to food, medication, and lifestyle factors.
Without a structured workflow, integrating CGM into clinical practice can create operational challenges. With the right support, including platforms like Theia, providers can streamline patient monitoring, improve clinical decision-making, and scale CGM programs effectively.
Providers looking to optimize their CGM workflow for providers will find that Theia’s platform supports efficient data review, patient engagement, and clinical interventions.
Moreover, using CGM in you nutrition practice enhances personalization and empowers patients to better manage their metabolic health through real-time feedback.
Interested in learning whether Theia is a fit for your practice? Book a call with our team